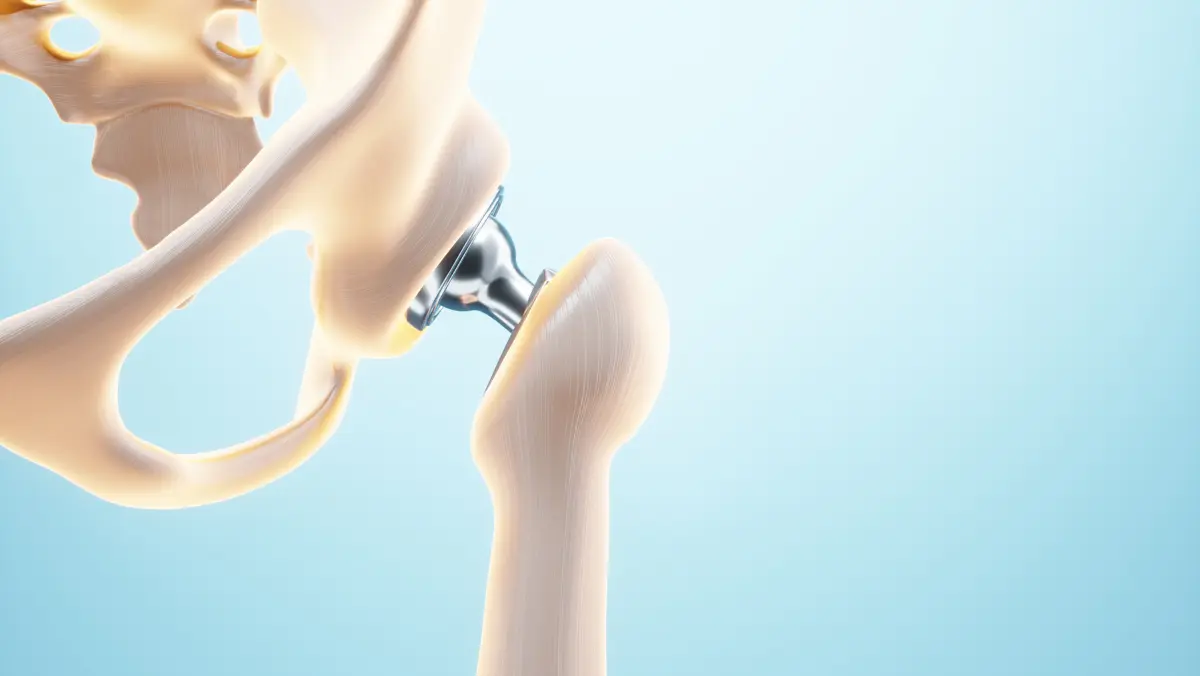
Arthroscopic trochanteric bursectomy in Chennai is a minimally invasive surgical procedure that is performed to remove the inflamed bursa sac in the hip. The trochanteric bursa is a small fluid-filled sac located on the side of the hip that acts as a cushion between the bone and the overlying soft tissues. The bursa can become inflamed due to trauma, overuse, or other medical conditions, leading to a condition called trochanteric bursitis.
The goal of arthroscopic trochanteric bursectomy in Chennai is to remove the inflamed bursa sac and any other damaged tissue in the area to relieve pain and improve hip function. The procedure is performed using a small camera called an arthroscope and specialized instruments inserted through small incisions in the skin. This minimally invasive approach allows for a quicker recovery time and reduced risk of complications compared to traditional open surgery.
Arthroscopic trochanteric bursectomy in Chennai is typically recommended when conservative treatments such as rest, ice, physical therapy, and medications have failed to provide relief. It is usually performed on an outpatient basis, and patients can typically resume normal activities within a few weeks of the procedure. Rehabilitation exercises are usually prescribed to help restore strength and mobility to the hip joint.
Arthroscopic Trochanteric Bursectomy in Chennai is a minimally invasive surgical procedure that is performed to treat shoulder impingement syndrome. Impingement syndrome occurs when the tendons or bursa in the shoulder become pinched or compressed as they pass through a narrow space between the bones and soft tissues of the shoulder joint. This can cause pain, inflammation, and limited range of motion in the shoulder.
During the arthroscopic decompression of impingement procedure, the surgeon will make a small incision in the shoulder and insert an arthroscope, which is a small camera that allows the surgeon to see inside the joint. The surgeon will then use specialized surgical instruments to remove any bony spurs or other obstructions that are causing the impingement. The procedure is typically performed on an outpatient basis, and patients can usually return to normal activities within a few weeks.
Arthroscopic decompression of impingement is considered to be a safe and effective treatment for shoulder impingement syndrome, and it has a high success rate. It is often recommended for patients who have not responded to conservative treatments such as rest, physical therapy, and medication.
Before undergoing arthroscopic decompression of impingement, the patient will typically undergo a thorough medical evaluation, including a review of their medical history and any current medications. The surgeon may also order imaging tests such as X-rays or MRI to assess the severity and location of the impingement.
The patient will be advised to stop taking any medications or supplements that may increase the risk of bleeding, such as aspirin, ibuprofen, or blood thinners, several days before the procedure. The patient will also need to fast for several hours before the surgery, typically starting at midnight on the day of the procedure.
The surgeon will discuss the risks and benefits of the procedure with the patient, including the potential for complications such as infection, bleeding, nerve damage, or continued pain. The patient will also be given specific instructions on how to prepare for the surgery, including when to arrive at the hospital or surgery center and what to bring with them.
Finally, the patient will need to arrange for transportation to and from the hospital or surgery center on the day of the procedure, as they will not be able to drive themselves home.
Arthroscopic decompression of impingement is a minimally invasive surgical procedure that is used to treat impingement syndrome, a condition in which the rotator cuff tendons or bursa become compressed and inflamed due to the narrowing of the subacromial space in the shoulder. The goal of the procedure is to relieve pain and restore the normal function of the shoulder joint.
The procedure is usually performed under general anesthesia on an outpatient basis. The surgeon will make several small incisions around the shoulder joint and insert an arthroscope, a thin, flexible tube with a camera on the end, to view the inside of the joint. The surgeon will then use special instruments to remove any bone spurs, inflamed tissue, or other obstructions that are causing the impingement. The procedure usually takes about 30-45 minutes.
After the surgery, the patient will be monitored in the recovery room before being discharged home the same day. The patient will be given pain medications and instructions on how to care for the incisions and manage pain. Physical therapy will usually begin within a few days to a week after the surgery to help restore strength and flexibility to the shoulder joint.
Arthroscopic decompression of impingement is generally a safe and effective procedure, with a high success rate and low risk of complications. However, as with any surgery, there are risks associated with the procedure, including infection, bleeding, nerve damage, and stiffness or weakness in the shoulder joint. These risks will be discussed with the patient prior to the surgery.
After arthroscopic decompression of impingement, patients typically experience postoperative pain and swelling. The level of pain and swelling varies from patient to patient and is dependent on several factors such as the extent of the impingement, the duration of the impingement, and the patient’s general health. Typically, the pain is most intense in the first few days after the procedure, and it can be controlled using pain medications and ice packs.
Patients may also experience some stiffness and limited mobility in the shoulder for a few weeks after the surgery. The surgeon may prescribe physical therapy to help restore the range of motion and strength of the shoulder joint.
It is important to keep the incision site clean and dry to prevent infection. Patients should follow the surgeon’s instructions on postoperative care, including changing the dressing, keeping the wound dry, and avoiding activities that may put stress on the shoulder joint.
Most patients can resume light activities within a few days after the procedure but should avoid heavy lifting or strenuous activities for several weeks. The surgeon will advise when it is safe to resume normal activities and when the patient can return to work or sports activities.
The recovery period after arthroscopic decompression of impingement can vary from patient to patient. Some patients may experience a full recovery within a few weeks, while others may take several months to return to full strength and range of motion. Compliance with postoperative care instructions and physical therapy is essential for successful rehabilitation.
Rehabilitation following arthroscopic decompression of impingement is crucial to ensure proper healing of the shoulder joint and to restore normal function. The rehabilitation protocol generally consists of several phases, each with specific goals and exercises.
The goal of the first phase is to protect the surgical site and allow for proper healing. During this phase, the arm is placed in a sling and the patient is instructed to perform gentle pendulum exercises and passive range of motion exercises. Active range of motion exercises are typically avoided during this phase.
The focus of the second phase is to gradually increase the range of motion of the shoulder and to improve strength. The patient is instructed to perform active assisted range of motion exercises with the assistance of a physical therapist or with the help of a pulley system. Strengthening exercises for the rotator cuff and scapular stabilizers are also introduced.
The third phase is designed to further improve shoulder strength, stability, and proprioception. Exercises such as plyometrics, resistance band exercises, and proprioceptive training are incorporated to improve the patient’s overall function.
The final phase focuses on returning the patient to their pre-injury level of activity. This includes sport-specific exercises and drills, as well as continued strengthening and range of motion exercises.
It is important for the patient to closely follow the rehabilitation protocol and work closely with their physical therapist to ensure proper healing and a successful outcome.
New No. 85, Royapettah High Road, Royapettah, Chennai – 600014
© Designed and Developed By cloudstar.digital