Arthroscopic-assisted Medial Patellofemoral Ligament (MPFL) Reconstruction is a surgical procedure used to treat patellar instability caused by a damaged or torn MPFL. The MPFL is a band of tissue that connects the femur (thigh bone) to the patella (kneecap) and helps keep the kneecap in place.
During the Arthroscopic assisted MPFL Reconstruction in Chennai, the surgeon will make small incisions around the knee joint and use a camera and specialized instruments to visualize and access the area. The damaged or torn MPFL is then removed and replaced with a graft from another part of the patient’s body or from a donor.
Arthroscopic assisted MPFL Reconstruction in Chennai is a minimally invasive procedure that has become more popular over time due to its high success rate, shorter recovery time, and reduced risk of complications compared to traditional open surgery. This procedure is typically performed on an outpatient basis, and most patients can return to their normal activities within a few months with proper rehabilitation.
As with any surgical procedure, you can expect certain risks such as bleeding, infection, and nerve damage. Patients should discuss the potential risks and benefits of this Arthroscopic assisted MPFL Reconstruction in Chennai with their surgeon before deciding if it is right for them.
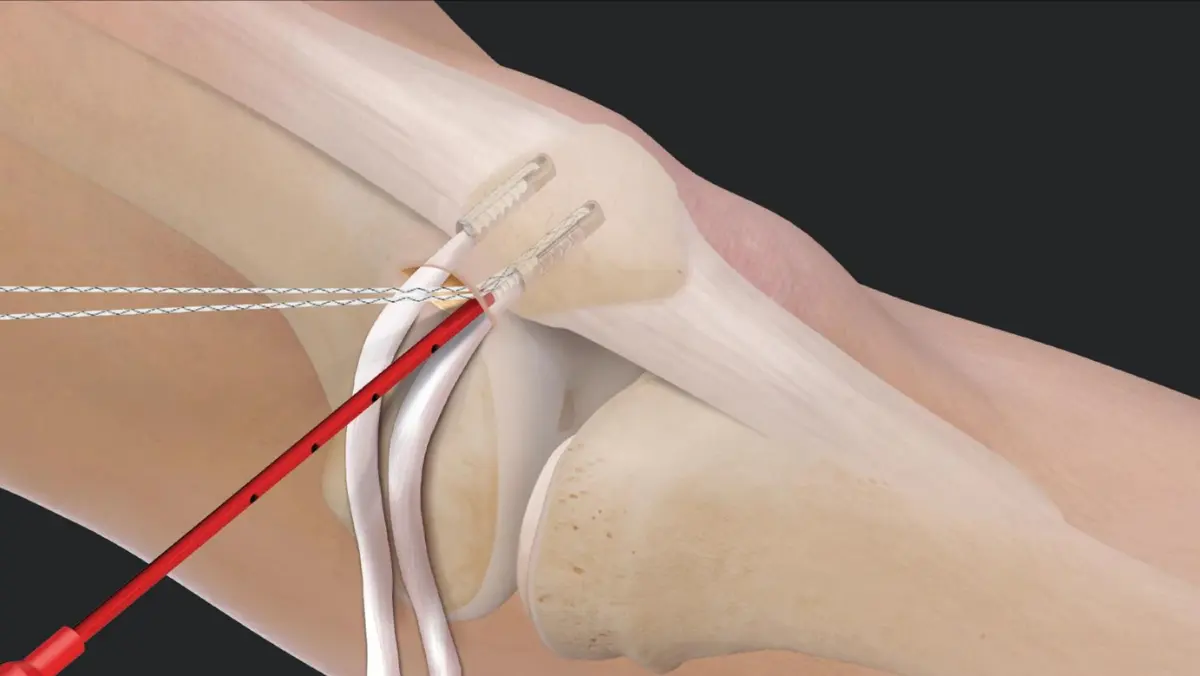
Arthroscopic-assisted Medial Patellofemoral Ligament (MPFL) Reconstruction is a surgical procedure that is performed to treat patellar instability. The MPFL is a ligament on the medial (inner) side of the knee that helps to stabilize the patella (kneecap) and prevent it from dislocating or shifting out of place.
When this ligament is damaged or torn, it can result in patellar instability, which can cause pain, swelling, and difficulty with normal activities such as walking, running, or climbing stairs. This is why Arthroscopic assisted MPFL Reconstruction in Chennai has to be performed.
Arthroscopic assisted MPFL Reconstruction in Chennai involves using minimally invasive techniques to reconstruct the damaged MPFL ligament. During the procedure, a small incision is made on the inner side of the knee, and an arthroscope (a thin, flexible tube with a camera and light source) is inserted to allow the surgeon to see inside the knee joint. The surgeon then uses a graft (a piece of tendon or ligament from another part of the body or a donor) to reconstruct the damaged MPFL ligament.
The surgical procedure of Arthroscopic assisted MPFL Reconstruction in Chennai is typically performed on an outpatient basis, meaning that the patient can go home on the same day as the surgery. After the procedure, a period of rehabilitation is necessary to help restore strength and function to the knee joint.
Before undergoing arthroscopic assisted MPFL reconstruction in Chennai, the patient will need to undergo a thorough evaluation and preparation process. This may involve a physical examination, imaging tests such as MRI or X-rays, and a review of the patient’s medical history and current medications. The patient may also need to stop taking certain medications, such as blood thinners, in the days leading up to the procedure.
Additionally, the surgeon may provide instructions on how to prepare the surgical site, such as shaving the area or applying an antiseptic solution. Finally, the patient may need to arrange for transportation to and from the hospital or surgical center on the day of the procedure.
Arthroscopic assisted MPFL reconstruction in Chennai is performed as an outpatient procedure under general anesthesia. The surgeon will make a few small incisions around the knee joint to insert the arthroscope and surgical instruments. The arthroscope will allow the surgeon to visualize the inside of the knee joint and assess the extent of the injury.
During the procedure, the surgeon will harvest a graft from the patient’s hamstring or patellar tendon, which will be used to reconstruct the MPFL. The graft will be passed through tunnels drilled in the femur and patella bones, and then secured in place with screws or sutures.
Once the graft is secured, the surgeon will confirm that the new ligament functions properly by testing the range of motion and stability of the knee joint. The incisions will then be closed, and a dressing and bandages will be applied to the knee. The patient will be moved to the recovery room to awaken from anesthesia and monitored for any complications.
After arthroscopic assisted MPFL reconstruction, the patient will be taken to the recovery room to wake up from anesthesia. Pain management and monitoring of vital signs will continue. The patient may also have a brace or splint on their knee, which will be adjusted accordingly by the medical staff.
The patient will be advised to keep their leg elevated and apply ice packs to reduce swelling. Pain medication and anti-inflammatory medication will be prescribed to manage pain and swelling.
The length of the hospital stay will depend on the individual patient and the extent of the surgery. Some patients may be discharged the same day, while others may need to stay overnight or for a few days.
The medical staff will provide detailed instructions on wound care, medication management, and rehabilitation exercises that should be followed post-surgery. Follow-up appointments will also be scheduled to monitor progress and make any necessary adjustments to the treatment plan.
Rehabilitation following an arthroscopic assisted MPFL reconstruction in Chennai typically involves a progressive and tailored program that is designed to help the patient recover full strength, range of motion, and function of the affected knee. The rehabilitation process is crucial for the success of the procedure and typically involves a combination of exercises, physical therapy, and lifestyle changes.
In the early stages of rehabilitation, patients are typically advised to limit weight-bearing activities and use crutches to avoid putting too much pressure on the affected knee. Physical therapy usually begins a few days after surgery and focuses on improving the range of motion and strengthening the muscles around the knee joint.
As the healing process progresses, patients will be gradually introduced to more challenging exercises to improve balance, coordination, and stability. Exercises such as squats, lunges, and leg presses are often included in the rehabilitation program to improve leg strength.
The length of the rehabilitation process varies from patient to patient and depends on factors such as age, overall health, and the extent of the surgery. On average, it can take anywhere from 3 to 6 months to fully recover from an arthroscopic assisted MPFL reconstruction in Chennai.
It is important to follow the rehabilitation program closely and attend all scheduled physical therapy sessions to ensure a successful outcome. Patients should also be mindful of their diet and avoid any activities that could put excessive strain on the affected knee, such as running or jumping, until they are cleared by their surgeon or physical therapist.
The recovery period following arthroscopic MPFL (Medial Patellofemoral Ligament) reconstruction can vary but typically ranges from 4 to 6 months. During this time, patients will undergo physical therapy to regain strength and flexibility in the knee, gradually returning to normal activities. Full recovery may take longer for some individuals, and it’s important to follow the surgeon’s post-operative instructions for the best outcome and to prevent re-injury.
Potential risks of arthroscopic MPFL reconstruction include infection, bleeding, nerve damage, and adverse reactions to anesthesia. There is also a small risk of graft failure or persistent instability. As with any surgical procedure, there is a possibility of scarring and the need for further surgery. It’s essential for patients to discuss these risks with their surgeon and consider their individual circumstances before deciding on the procedure.
Medial Patellofemoral Ligament (MPFL) reconstruction can significantly reduce the risk of future patellar dislocations. This procedure stabilizes the kneecap, preventing it from slipping out of place. However, it’s not a guarantee against all future dislocations, as other factors and injuries can play a role. Successful rehabilitation, adherence to post-operative care, and physical therapy are crucial for optimizing the procedure’s effectiveness and reducing the likelihood of recurring dislocations.
New No. 85, Royapettah High Road, Royapettah, Chennai – 600014
© Designed and Developed By cloudstar.digital